A missing tooth can change more than a smile. It can shift the bite, alter speech, and make simple meals feel like a chore. Many people also start chewing on one side, which strains the jaw and wears down the remaining teeth faster. The good news is that modern tooth replacement can restore both function and comfort in a way that feels stable and natural.
In many practices, including Orto Nova dental implants, the focus stays on long-term results, not quick fixes. That means careful planning, realistic expectations, and a step-by-step process built around bone health, gum stability, and a bite that works in everyday life.
What a Dental Implant Actually is And Why It Feels So Stable
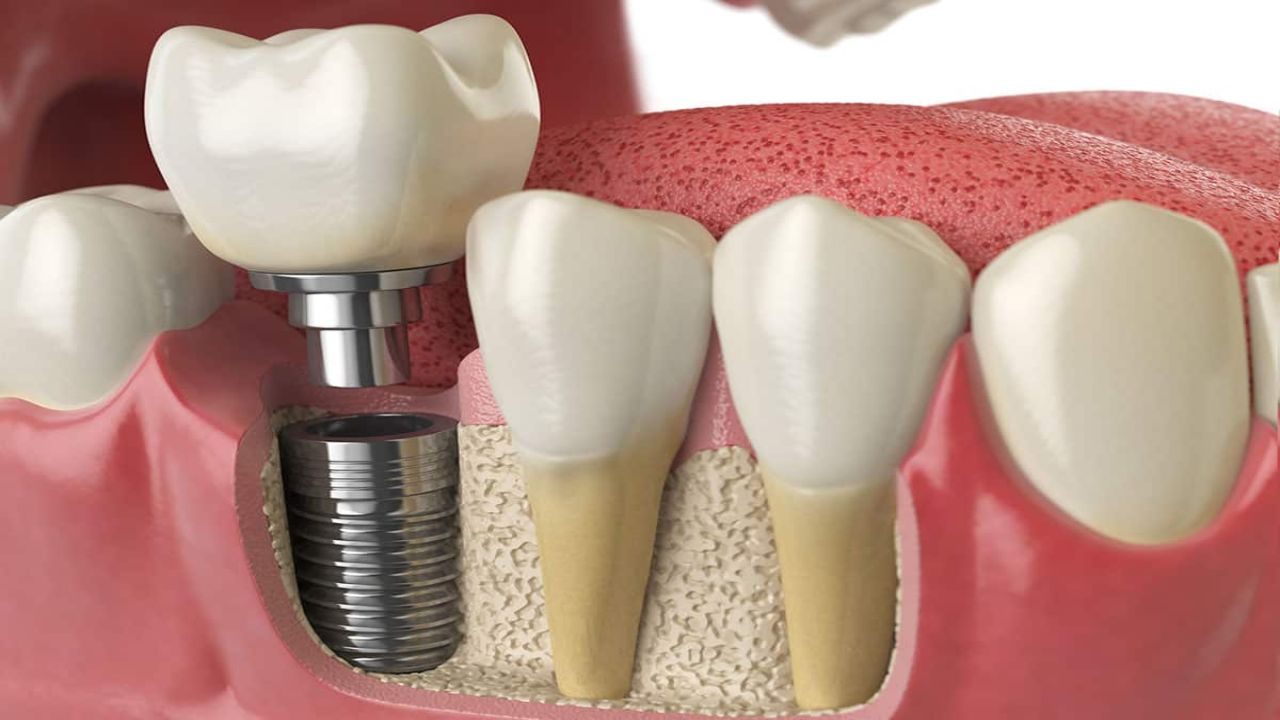
A dental implant works like a new tooth root. The dentist places a small post, most often titanium or a titanium alloy, into the jawbone. This post does not sit “on top” of the gums like a removable appliance. It anchors into the bone, which gives the final tooth replacement its firm, secure feel during chewing and speaking.
After placement, the bone begins to fuse to the implant surface in a process called osseointegration. Think of it as a biological handshake between living bone and a highly compatible surface. This connection matters because it turns the implant into a true foundation. When the final crown or bridge attaches later, the chewing forces travel through the implant into the jaw, similar to a natural tooth.
Implants also help protect the shape of the jaw. When a tooth goes missing, the bone in that area can shrink over time because it no longer receives regular chewing stimulation. An implant can help maintain that stimulation, supporting facial structure and reducing the sunken look that sometimes follows tooth loss.
The Step-by-Step Process from Consultation to Final Tooth
The process starts with a planning visit, not a drill. A dentist reviews your medical history, evaluates gum health, and checks how your teeth meet when you bite. Most offices use 3D imaging to measure bone volume and map key anatomy. This planning stage guides implant size, position, and angle so the final tooth looks right and functions cleanly.
Next comes implant placement. The dentist numbs the area and creates a precise site in the bone for the implant. Many patients feel pressure but little pain during the procedure. After placement, the gums heal while the bone begins its bonding phase. Some cases allow a temporary tooth during healing, while others need a short period without a visible tooth, depending on stability and bite forces.
After healing, the dentist connects a small component called an abutment, which links the implant to the visible tooth. Then the final crown, bridge, or denture attaches. The key point is balance. The dentist checks the bite carefully so the implant restoration avoids excessive stress and blends smoothly with the surrounding teeth.
Osseointegration Explained in Plain Language
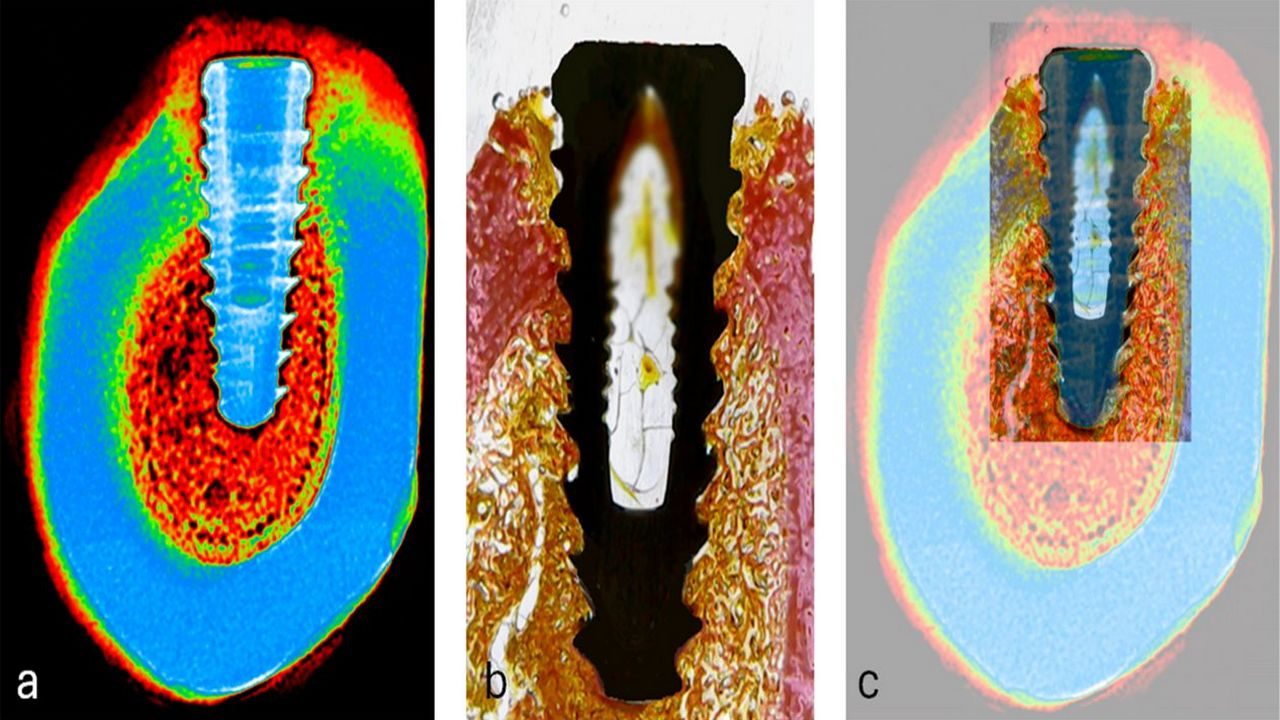
Osseointegration sounds technical, but the idea stays simple. Your bone cells grow and remodel around the implant surface until they form a tight bond. This bond provides the strength that lets an implant support real chewing forces, not just light cosmetic use.
Several factors influence how smoothly this stage goes. Bone density matters, and so does overall health. Smoking can slow healing. Uncontrolled diabetes can raise infection risk and reduce healing quality. Grinding or clenching can overload the implant early if a patient does not use a night guard when needed. A good provider plans around these realities instead of hoping they disappear.
Time also plays a role. Some implants stabilize faster, while others need more healing time. Your dentist will choose the timeline based on stability at placement, bone conditions, and the type of restoration planned. A careful pace can feel slower in the moment, but it often protects results for years.
Materials, Design, and the Parts That Make Implants Work
Most implants use titanium because the body accepts it well and bone bonds to it predictably. Some systems use zirconia, a ceramic material that matches tooth color and can work well for select cases. The right material depends on anatomy, gum thickness, bite forces, and aesthetic goals. A skilled dentist will explain options in plain language and match the system to your needs.
An implant restoration has three core parts: the implant post in the bone, the abutment above the gumline, and the crown or prosthetic tooth on top. The abutment can be stock or custom-made. Custom abutments often help in visible areas because they shape the gumline and support a natural emergence profile, meaning the tooth appears to “grow” from the gums like a real tooth.
Design details also matter more than most people expect. Implant surface texture can influence bone bonding. Implant diameter and length affect stability. Even the placement angle can impact how easy it is to clean. Great results come from small technical decisions that protect bite balance, gum health, and long-term maintenance.
Who is a Strong Candidate and What Can Improve Eligibility

Many adults qualify for implants, but the dentist must confirm three essentials: healthy gums, enough bone to support the implant, and a stable plan for oral hygiene. If gum disease exists, treatment must come first. Inflamed gums can compromise healing and raise the risk of implant complications down the road.
Bone quantity and quality also count. If the jaw has thinned after tooth loss, bone grafting may help rebuild the area. A graft sounds intimidating, but many grafts involve a small amount of bone material placed to support new growth. Sinus lift procedures can also create more space for implants in the upper back jaw. These steps can expand eligibility for patients who assumed they had “missed the window.”
Lifestyle factors can change outcomes, too. Smoking, heavy grinding, and inconsistent brushing can shorten the lifespan of any restoration, including implants. On the other hand, patients who keep regular cleanings, manage medical conditions, and follow bite-protection advice often enjoy very stable results.
Recovery, Aftercare, and How to Protect Results for the Long Term
Recovery tends to feel manageable for most patients. Mild swelling and soreness can show up for a few days, especially after multiple implants or grafting. Dentists often recommend soft foods, careful brushing near the area, and avoiding straws early on. Pain control usually relies on standard anti-inflammatory medicine unless the case requires something stronger.
After the final tooth is in place, aftercare becomes the real secret to longevity. Implants cannot get cavities, but the gums around them can still inflame. That condition, called peri-implant mucositis, can progress if plaque builds up. Daily brushing, interdental cleaning, and regular professional visits keep the tissue healthy and reduce risk.
Long-term protection also includes bite awareness. If you clench or grind, a night guard can prevent excessive forces that stress the implant and the surrounding bone. Many implant problems trace back to overload and poor cleaning habits, not “implant failure” in the dramatic sense. With steady care and good follow-up, implants can support confident chewing, clearer speech, and a smile that feels like your own again.

